
A Case Report: Combined Acupuncture and Low-Level Laser Therapy to Mitigate Radiation-induced Oral Mucositis
Introduction
Oral mucositis is one of the most common forms of side effects in patients undergoing radiation therapy on the head and neck (H&N) (American Cancer Society, 2020). Globally, there are 890,000 new cases (4.5% of all cancers) every year of H&N squamous cell carcinoma (Barsouk et al., 2023). An estimated 80-100% of patients who undergo radiation therapy have to manage its side effects (Cleveland Clinic, 2022).
Radiation therapy is the standard form of H&N cancer treatment to target specific areas, especially post-surgery, to kill lingering cancer cells (Radiation, 2019). High doses of energy damage the DNA of cancer cells, interrupting replication, however, this also injures healthy cells (National Cancer Institute, 2019). H&N radiation degrades the mucosal lining of the oral cavity, as well as the taste buds, making oral mucositis and dysgeusia (altered taste) the most common side effects. Oral mucositis can encompass symptoms such as a red, swollen mouth or gums, xerostomia (dry mouth), mouth ulcers, pain, difficulty swallowing, and bleeding (Cleveland Clinic, 2022).
Small trials and pilot studies (Garcia et al., 2009; Blom et al., 1996) show that acupuncture may relieve radiation-induced xerostomia, possibly via stimulation of salivary gland activity. However, until recently, few rigorously controlled trials had tested acupuncture in long‐term head and neck cancer survivors with chronic post-radiation symptoms. The evidence remains limited, particularly with respect to objective salivary flow measures and outcomes such as dysgeusia.
Low-level laser therapy (LLLT) is another modality that is used to improve salivation and decrease the severity of mucositis (González-Arriagada et al., 2017). It is hypothesized that LLLT may stimulate residual gland function in addition to its other known functions such as improving microcirculation, increasing cell respiration, and enhancing ATP production (Palma et al., 2017).
This case report examines the treatment of a 70-year-old female who underwent radiation therapy for tonsillar cancer. Her symptoms included oral pain, xerostomia, and dysgeusia, treated with acupuncture for three years and laser therapy for one year, with significant patient-reported benefit. Given the limited research on acupuncture for the side effects of H&N radiation, this case study aims to provide insight and an avenue for further investigation.
Diagnostic Theory
Yin is the material substance of the body that keeps things moist and nourished. Radiation therapy introduces toxic heat to the body, especially the upper burner, which dessicates yin substances such as body fluids resulting in symptoms like dry mouth, dry skin, skin burns, and dysphagia (Li et al., 2003; Ding, 2021; Maciocia, 2003).
Liver and Kidney yin deficiency due to toxic heat invasion is the most common diagnosis for patients undergoing radiation therapy (Wang, 2023). Liver yin and Kidney yin are closely related to one another, so when one of them is depleted, the other soon will be as well (Ding, 2021). Furthermore, yin deficiency due to toxic heat can lead to both qi and blood deficiency because blood is a yin substance, and blood is the mother of qi, which means it carries and nourishes qi (Ding, 2021). When there is insufficient blood, qi becomes deficient, most often Spleen qi, which can be observed in the poor appetite and fatigue of patients undergoing radiation and chemotherapy (Wang, 2023). When Spleen qi is deficient, it also fails to support the Lung in sending body fluids upward, resulting in diminished saliva (Li et al., 2003; Maciocia, 2003).
Patient Information
The patient was a 70-year-old Caucasian female presenting with the chief complaint of oral mucositis. She was diagnosed with tonsillar cancer in 2020 and has been dealing with dysgeusia, xerostomia, and oral pain ever since undergoing radiation and chemotherapy.
Cancer symptoms started as a persistent earache, found to be caused by a 3 cm nodule in her throat. Surgery removed the surrounding lymph nodes and the cancer entirely in July 2020. Radiation therapy until September 2020 targeted the remaining surrounding lymph nodes.
During this process, the patient developed mouth pain, xerostomia, and dysgeusia; the only foods she could tolerate were bananas and lemons. She was often fatigued, and the severity of dryness limited her to a liquid diet. She lost ~50 lbs.. Intermittent thrush was treated with nystatin. Her extensive medical history and medication list may be seen in Table 1 and Appendix A.
Table 1. List of medical conditions
At her initial intake, her tongue was dry and dark red in color, with horizontal fissures branching from a deep vertical fissure. Additionally, she had a peeled tongue coating, a sign of severe yin deficiency. Pulse assessment revealed a weak and thready pulse.
Throughout her year of treatment, her tongue alternated between a deep red and pale color, and from a geographic to a peeled coating, but the fissures always remained, though the lessening in depth. Yin deficiency and Spleen qi deficiency were her most common TCM diagnoses, considering all the dryness she had as well as dysgeusia, recurrent infection, and fatigue.
Treatment
The patient received a total of 45 treatments from Spring 2021 to Fall 2024. Consistent laser therapy began during the last 21 treatments, from Spring 2023 to Fall 2024. Before beginning LLLT, the patient confirmed that she was cancer free in the head and neck area, since LLLT may be contraindicated for active tumor sites (Bamps, 2018).
Acupuncture students from Bastyr University provided care under the supervision of licensed acupuncturists at the Bastyr Center of Natural Health in Seattle, Washington. Acupuncture treatments were dependent on each supervisor and student, but points were selected based on TCM principles.
The patient had private acupuncture until Treatment 14, then switched to a community acupuncture setting. Needle retention time ranged from 20 in private sessions to 45 minutes in community acupuncture. Seiren D-Type needles were used for Yintang, and for other points, Mac 36 and 34 gauge, 30 mm needles were inserted to the appropriate depth with minimal stimulation.
Infrared (IR) LLLT was performed with an Advant LZ30k laser using the acupuncture probe head protected with plastic wrap. Touching the tongue, the laser was moved slowly over the affected areas. Dosages and settings varied slightly between treatments.
Table 2: List of acupuncture treatments and point selections
Treatment Outcomes
A visual analog scale (VAS), 1-10, with 10 being the worst, was used for the first 14 treatments. During the first treatment, the patient reported a pain level of 10/10 without the use of pain medication and 6/10 with the use of pain medication.
As mentioned, pain limited her diet to milk, bananas, smoothies, and cereals, which had to be washed down with a liquid. Fatty foods, sweets, eggs, and cheese tasted rancid, while fruits would burn her tongue. She had episodes of high pain (10/10) and dysgeusia due to eating spicy or acidic foods (except for lemon), but the pain would decrease and stabilize after a week or post-treatment. Her pain stabilized to 2-3/10 from treatments 4-12. The pain increased to 6/10 during Treatment 13 and reduced to 4/10 during Treatment 14. By Treatment 21, she reported a decrease in dysgeusia and could eat apples, one of the most challenging foods previously.
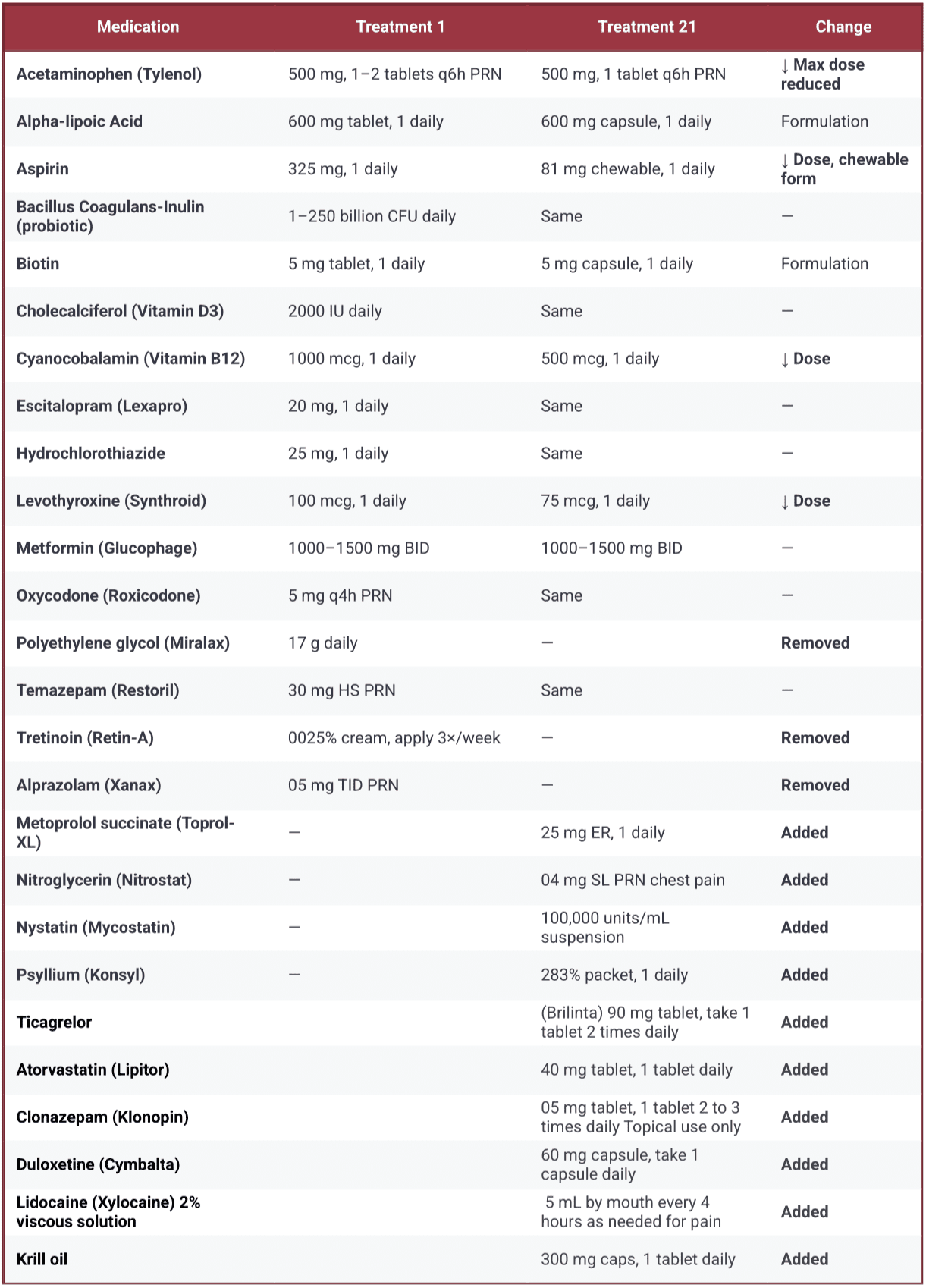
As can be seen in Appendix A, although the medication list increased overall, her pain medication list stayed relatively the same. The dose and frequency of the pain medication slightly decreased over time. Acetaminophen was then taken once a day as opposed to every 6 hrs; aspirin decreased from 325mg to 81mg, and oxycodone was taken every 6 instead of every 4 hrs.
Between Treatments 17 and 18, the patient came to the clinic to receive treatment, even though she knew she had to go to urgent care due to a large hematoma from a fall. She said she did not want to miss an appointment because the LLLT and acupuncture helped her dry mouth and pain so much.
The most improvement was observed during treatments administered in close succession. The pain level between treatment 9 (week 16) and treatment 10 (week 34) remained the same, which may be due to the combination of treatments and medication that she started during treatment 5 (week 10).
From the onset of the tonsillar cancer, the patient weighed 180 lb in the spring of 2020. When she started acupuncture in 2021 without LLLT, she weighed 146 pounds. By the time she started LLLT in combination with acupuncture in the spring of 2023, she weighed 126 lb, and by the fall of 2024, she weighed 133 lb. Her weight fluctuated between 126 lb and 133 lb throughout 2023 and 2024, but it remained steady, and she did not experience the same weight loss as she had between 2020 and 2022.
Figure 1: In-office VAS scale per treatment up until Treatment 14
Episodic pain would reach 10/10 between treatments. Figure 2: In-office VAS per treatment based on weeks up until Treatment 14 Episodic pain would reach 10/10 between treatments.Discussion
The side effects of H&N radiation therapy can be long-lasting. There has been some controversy on the benefit of acupuncture for people experiencing xerostomia, stating there is insufficient evidence (Assy & Brand, 2018). There has been recent research on acupuncture to help alleviate these symptoms (Regina de Sousa et al., 2023), which involves stimulating the salivary glands and using other body and auricular points.
LLLT also shows promise in treating radiation-induced xerostomia, depending on the type of protocol used (Ribeiro et al., 2024). There have been more recent studies on LLLT and acupuncture as separate modalities to improve symptoms of oral mucositis; however, no studies have combined the two modalities. The closest study investigated the effects of laser acupuncture on salivary flow rate in individuals with Sjögren's syndrome, revealing a significantly higher production of saliva (Cafaro et al., 2014). The control group did not receive manual acupuncture.
This case report highlights the potential benefits of acupuncture and LLLT treatment in stabilizing patients experiencing oral mucositis, thereby improving their quality of life and alleviating symptoms of oral mucositis. From a biomedical perspective, the mechanisms of acupuncture are not well understood; however, it is hypothesized that acupuncture affects the central nervous system by manipulating the fascia and increasing blood flow both locally and distally, thereby stimulating saliva production (Cohen et al., 2024). LLLT has been shown to upregulate ATP production, facilitating tissue repair, and has an analgesic effect by releasing endorphins (Dantas et al., 2020).
From a TCM perspective, this patient had xerostomia and dysgeusia caused by severe yin and Spleen qi deficiency. It can be hypothesized that tonifying the yin reduced the fissures in the tongue. Also, from tonifying the Stomach and Spleen qi, a tongue coat was able to form (Ding, 2021). It is unlikely that needles alone would have strengthened yin directly, because yin is a physical substance requiring tangible nourishment from diet and herbs (Williams, 2024). This patient's food restriction made supporting yin particularly difficult. However, acupuncture can be used to tonify qi, and by tonifying qi, it can in turn generate blood, which nourishes yin (Ding, 2021).
Improving sleep quality can also nourish blood and yin (Williams, 2024). Although the interpretation of LLLT in TCM terms has not been researched, clinically, it appears to tonify qi and yang. It is contradictory that LLLT does not introduce more heat, which can be detrimental to the body. However, it is similar to moxibustion in that it introduces heat into the body to warm yang and tonify qi.
This case was complicated by recurrent candida infections that aggravated the oral mucositis. Although inconsistent, during the periods the patient was receiving more weekly treatment, her pain stabilized, and she reported that the treatments were helping prevent the pain and xerostomia from surging back. An in vitro study investigating LLLT for oral candida resulted in a reduction of colonies; however, further research is needed to confirm their findings (Hasanah et al., 2024). Despite that, the study suggests LLLT may help alleviate oral pain by reducing candida infection in combination with nystatin.
It is important to consider the limitations of this case. Due to multiple students charting, it became difficult to track the patient's progress quantitatively, as the VAS was missing for the last seven treatments, and the forms of treatment kept changing depending on the supervisor. The acupuncture points used and the LLLT settings and amounts of joules applied to the tongue varied inconsistently throughout the treatments. The VAS score was also affected by having different clinicians, as well as the patient normalizing her new standard pain tolerance to 3/10. There were multiple instances where she reported having increased pain and being unable to eat, but she reported on average a 3/10 in office.
Additionally, there was no device to measure the amount of saliva she was producing. The follow-up was also not consistent. The timing of each treatment was spread apart, and information such as diet change and severity of oral mucositis was sometimes absent. No adverse reactions for acupuncture or LLLT were reported.
Conclusion
This case report examines the potential benefits of combining acupuncture and LLLT in treating oral mucositis in patients who have undergone head and neck radiation. Although this case study has many limitations, it provides insight into methods to improve the quality of life, pain, and xerostomia associated with radiation-induced oral mucositis.
Informed Consent
The patient provided written informed consent for the publication of this case report, and a copy is on file with the author.
Safety
No adverse events were anticipated or reported.
ResourcesAmerican Cancer Society. (2020). Side effects of radiation therapy. https://www.cancer.org/cancer/managing-cancer/treatment-types/radiation/effects-on-different-parts-of-body.html
Assy, Z., & Brand, H. S. (2018). A systematic review of the effects of acupuncture on xerostomia and hyposalivation. BMC Complementary and Alternative Medicine, 18(1), 57. https://doi.org/10.1186/s12906-018-2123-8
Bamps, M., Dok, R., & Nuyts, S. (2018). Low-level laser therapy stimulates proliferation in head and neck squamous cell carcinoma cells. Frontiers in Oncology, 8, 343. https://doi.org/10.3389/fonc.2018.00343
Barsouk, A., Aluru, J. S., Rawla, P., Saginala, K., & Barsouk, A. (2023). Epidemiology, risk factors, and prevention of head and neck squamous cell carcinoma. Medical Sciences, 11(2), 42. https://doi.org/10.3390/medsci11020042
Blom, M., Dawidson, I., Fernberg, J., Johnson, G., & Angmar-Månsson, B. (1996). Acupuncture treatment of patients with radiation-induced xerostomia. European Journal of Cancer Part B: Oral Oncology, 32(3), 182–190. https://doi.org/10.1016/0964-1955(95)00099-2
Cafaro, A., Arduino, P. G., Gambino, A., Romagnoli, E., & Broccoletti, R. (2014). Effect of laser acupuncture on salivary flow rate in patients with Sjögren’s syndrome. Lasers in Medical Science, 30(4), 1805–1809. https://doi.org/10.1007/s10103-014-1631-1
Cleveland Clinic. (2022). Mucositis: Types, symptoms & treatment. https://my.clevelandclinic.org/health/diseases/24181-mucositis
Cohen, L., Danhauer, S. C., Garcia, M. K., Dressler, E. V., Rosenthal, D. I., Chambers, M. S., Cusimano, A., Brown, W. M., Ochoa, J. M., Yang, P., Chiang, J. S., Gordon, O., Crutcher, R., Kim, J. K., Russin, M. P., Lukenbill, J., Porosnicu, M., Yost, K. J., Weaver, K. E., & Lesser, G. J. (2024). Acupuncture for chronic radiation-induced xerostomia in head and neck cancer: A multicenter randomized clinical trial. JAMA Network Open, 7(5), e2410421. https://doi.org/10.1001/jamanetworkopen.2024.10421
Dantas, J. B. de L., Martins, G. B., Lima, H. R., Carrera, M., Reis, S. R. de A., & Medrado, A. R. A. P. (2020). Evaluation of preventive laser photobiomodulation in patients with head and neck cancer undergoing radiochemotherapy. Special Care in Dentistry, 40(4), 364–373. https://doi.org/10.1111/scd.12479
Ding, W. (2021). TCM fundamentals [Lecture presentation]. Seattle, WA, United States.
Garcia, M. K., Chiang, J. S., Cohen, L., Liu, M., Palmer, J. L., Rosenthal, D. I., Wei, Q., Tung, S., Wang, C., Rahlfs, T., & Chambers, M. S. (2009). Acupuncture for radiation-induced xerostomia in patients with cancer: A pilot study. Head & Neck, 31(10), 1360–1368. https://doi.org/10.1002/hed.21094
González-Arriagada, W. A., Ramos Innocentini, L. M., Andrade, M. A. C., & Lopes, M. A. (2018). Efficacy of low-level laser therapy as an auxiliary tool for management of acute side effects of head and neck radiotherapy. Journal of Cosmetic and Laser Therapy, 20(2), 117–121. https://doi.org/10.1080/14764172.2017.1376094
Hasanah, N. T., Sufiawati, I., Kusumadjati, A., & Sunardi, M. A. (2024). In vitro effect of low-level laser therapy on Candida albicans colonies isolated from patients undergoing radiotherapy for head and neck cancer. Journal of Lasers in Medical Sciences, 15, e11. https://doi.org/10.34172/jlms.2024.11
Li, P., Chen, Z., Du, X., & Maciocia, G. (2003). Management of cancer with Chinese medicine. Donica Publishing Ltd.
National Cancer Institute. (2019). Radiation therapy for cancer. https://www.cancer.gov/about-cancer/treatment/types/radiation-therapy
Palma, L. F., Gonnelli, F. A. S., Marcucci, M., Dias, R. S., Giordani, A. J., Segreto, R. A., & Segreto, H. R. C. (2017). Impact of low-level laser therapy on hyposalivation, salivary pH, and quality of life in head and neck cancer patients post-radiotherapy. Lasers in Medical Science, 32(4), 827–832. https://doi.org/10.1007/s10103-017-2182-4
Regina de Sousa, T. R., Mattos, S., Marcon, G., Furtado, T., & Duarte da Silva, M. (2023). Acupuncture techniques and acupoints used in individuals under chemotherapy or radiotherapy treatment of cancer: A systematic review. Journal of Clinical Nursing, 32(19–20), 6917–6933. https://doi.org/10.1111/jocn.16722
Ribeiro, L. N., de Vasconcelos Carvalho, M., de Oliveira Limirio, J. P. J., do Egito Vasconcelos, B. C., Moraes, S. L. D., & Pellizzer, E. P. (2024). Impact of low-level laser therapy on the quality of life of patients with xerostomia undergoing head and neck radiotherapy: A systematic review. Supportive Care in Cancer, 32(2), 118. https://doi.org/10.1007/s00520-023-07939-5
Wang, Y. (2023). Manage concurrent conditions [Lecture presentation]. Seattle, WA, United States.
Williams, C. (2024). Needles and yin: Beyond the kidney meridian.
Appendix A
Comparison of medications from first to last treatment. (Changes in medication frequency or dose are in bold.)
 OPEN ACCESS
OPEN ACCESS
Citation: Nguyen, P. (2025). A Case Report: Combined Acupuncture and
Low-Level Laser Therapy to Mitigate Radiation-induced Oral Mucositis. Convergent Points: An East-West Case Report Journal 4(2). www.convergentpoints.com
Editor: Kathleen Lumiere, Seattle Institute of East Asian Medicine, UNITED STATES
Received: March 19, 2025
Accepted: September 18, 2025
Published: October 15, 2025
Copyright: © 2025 Nguyen. This open-access article is distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Data Availability Statement: All relevant data are within the paper and its supporting information files.
Funding: This article received no funding of any type.
Competing Interests: The author has declared that no competing interests exist.
American Cancer Society. (2020). Side effects of radiation therapy. https://www.cancer.org/cancer/managing-cancer/treatment-types/radiation/effects-on-different-parts-of-body.html
Assy, Z., & Brand, H. S. (2018). A systematic review of the effects of acupuncture on xerostomia and hyposalivation. BMC Complementary and Alternative Medicine, 18(1), 57. https://doi.org/10.1186/s12906-018-2123-8
Bamps, M., Dok, R., & Nuyts, S. (2018). Low-level laser therapy stimulates proliferation in head and neck squamous cell carcinoma cells. Frontiers in Oncology, 8, 343. https://doi.org/10.3389/fonc.2018.00343
Barsouk, A., Aluru, J. S., Rawla, P., Saginala, K., & Barsouk, A. (2023). Epidemiology, risk factors, and prevention of head and neck squamous cell carcinoma. Medical Sciences, 11(2), 42. https://doi.org/10.3390/medsci11020042
Blom, M., Dawidson, I., Fernberg, J., Johnson, G., & Angmar-Månsson, B. (1996). Acupuncture treatment of patients with radiation-induced xerostomia. European Journal of Cancer Part B: Oral Oncology, 32(3), 182–190. https://doi.org/10.1016/0964-1955(95)00099-2
Cafaro, A., Arduino, P. G., Gambino, A., Romagnoli, E., & Broccoletti, R. (2014). Effect of laser acupuncture on salivary flow rate in patients with Sjögren’s syndrome. Lasers in Medical Science, 30(4), 1805–1809. https://doi.org/10.1007/s10103-014-1631-1
Cleveland Clinic. (2022). Mucositis: Types, symptoms & treatment. https://my.clevelandclinic.org/health/diseases/24181-mucositis
Cohen, L., Danhauer, S. C., Garcia, M. K., Dressler, E. V., Rosenthal, D. I., Chambers, M. S., Cusimano, A., Brown, W. M., Ochoa, J. M., Yang, P., Chiang, J. S., Gordon, O., Crutcher, R., Kim, J. K., Russin, M. P., Lukenbill, J., Porosnicu, M., Yost, K. J., Weaver, K. E., & Lesser, G. J. (2024). Acupuncture for chronic radiation-induced xerostomia in head and neck cancer: A multicenter randomized clinical trial. JAMA Network Open, 7(5), e2410421. https://doi.org/10.1001/jamanetworkopen.2024.10421
Dantas, J. B. de L., Martins, G. B., Lima, H. R., Carrera, M., Reis, S. R. de A., & Medrado, A. R. A. P. (2020). Evaluation of preventive laser photobiomodulation in patients with head and neck cancer undergoing radiochemotherapy. Special Care in Dentistry, 40(4), 364–373. https://doi.org/10.1111/scd.12479
Ding, W. (2021). TCM fundamentals [Lecture presentation]. Seattle, WA, United States.
Garcia, M. K., Chiang, J. S., Cohen, L., Liu, M., Palmer, J. L., Rosenthal, D. I., Wei, Q., Tung, S., Wang, C., Rahlfs, T., & Chambers, M. S. (2009). Acupuncture for radiation-induced xerostomia in patients with cancer: A pilot study. Head & Neck, 31(10), 1360–1368. https://doi.org/10.1002/hed.21094
González-Arriagada, W. A., Ramos Innocentini, L. M., Andrade, M. A. C., & Lopes, M. A. (2018). Efficacy of low-level laser therapy as an auxiliary tool for management of acute side effects of head and neck radiotherapy. Journal of Cosmetic and Laser Therapy, 20(2), 117–121. https://doi.org/10.1080/14764172.2017.1376094
Hasanah, N. T., Sufiawati, I., Kusumadjati, A., & Sunardi, M. A. (2024). In vitro effect of low-level laser therapy on Candida albicans colonies isolated from patients undergoing radiotherapy for head and neck cancer. Journal of Lasers in Medical Sciences, 15, e11. https://doi.org/10.34172/jlms.2024.11
Li, P., Chen, Z., Du, X., & Maciocia, G. (2003). Management of cancer with Chinese medicine. Donica Publishing Ltd.
National Cancer Institute. (2019). Radiation therapy for cancer. https://www.cancer.gov/about-cancer/treatment/types/radiation-therapy
Palma, L. F., Gonnelli, F. A. S., Marcucci, M., Dias, R. S., Giordani, A. J., Segreto, R. A., & Segreto, H. R. C. (2017). Impact of low-level laser therapy on hyposalivation, salivary pH, and quality of life in head and neck cancer patients post-radiotherapy. Lasers in Medical Science, 32(4), 827–832. https://doi.org/10.1007/s10103-017-2182-4
Regina de Sousa, T. R., Mattos, S., Marcon, G., Furtado, T., & Duarte da Silva, M. (2023). Acupuncture techniques and acupoints used in individuals under chemotherapy or radiotherapy treatment of cancer: A systematic review. Journal of Clinical Nursing, 32(19–20), 6917–6933. https://doi.org/10.1111/jocn.16722
Ribeiro, L. N., de Vasconcelos Carvalho, M., de Oliveira Limirio, J. P. J., do Egito Vasconcelos, B. C., Moraes, S. L. D., & Pellizzer, E. P. (2024). Impact of low-level laser therapy on the quality of life of patients with xerostomia undergoing head and neck radiotherapy: A systematic review. Supportive Care in Cancer, 32(2), 118. https://doi.org/10.1007/s00520-023-07939-5
Wang, Y. (2023). Manage concurrent conditions [Lecture presentation]. Seattle, WA, United States.
Williams, C. (2024). Needles and yin: Beyond the kidney meridian.
Appendix A
Comparison of medications from first to last treatment. (Changes in medication frequency or dose are in bold.)
Citation: Nguyen, P. (2025). A Case Report: Combined Acupuncture and Low-Level Laser Therapy to Mitigate Radiation-induced Oral Mucositis. Convergent Points: An East-West Case Report Journal 4(2). www.convergentpoints.com Editor: Kathleen Lumiere, Seattle Institute of East Asian Medicine, UNITED STATES Received: March 19, 2025 Accepted: September 18, 2025 Published: October 15, 2025 Copyright: © 2025 Nguyen. This open-access article is distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Data Availability Statement: All relevant data are within the paper and its supporting information files. Funding: This article received no funding of any type. Competing Interests: The author has declared that no competing interests exist. |